Hernia Surgery in Colombia – Dr. José Agámez
Anatomy-driven abdominal wall repair with minimally invasive and open options
Hernia surgery is not just about closing a defect.
From a clinical standpoint, it is about restoring abdominal wall integrity, reducing the risk of progression, and selecting the most appropriate repair strategy for each patient.
Not all hernias require the same operation, and not all patients benefit from the same approach. Surgical indication depends on the type of hernia, anatomical location, symptom burden, prior surgery, and overall risk–benefit profile.
This page covers the evaluation and treatment of inguinal, umbilical, ventral, and incisional hernias, including laparoscopic hernia repair, selected use of
robotic surgery in Colombia, and open techniques when they offer the safest and most durable reconstruction.
If you are exploring hernia surgery in Colombia, the goal is not to promise the same treatment for every defect, but to determine which repair strategy best matches the anatomy of the hernia and the functional needs of the abdominal wall. You can also explore my full range of
minimally invasive surgical services in Colombia
or learn more about Dr. José Agámez.
What is a hernia and when should it be repaired?
A hernia develops when part of the abdominal contents pushes through a weakness or defect in the fascia and muscular layers of the abdominal wall. From a clinical standpoint, this is not simply a visible bulge. It represents a structural loss of abdominal wall integrity that may progressively enlarge over time, especially with physical effort, coughing, increased intra-abdominal pressure, weight gain, or previous surgery.
Not all hernias behave in the same way. Some remain minimally symptomatic for a period of time, while others enlarge, become painful, or develop complications such as incarceration, bowel obstruction, or strangulation. Surgical indication depends on symptoms, anatomical location, defect size, progression over time, and the expected risk–benefit balance of repair. Not all patients require immediate surgery, but all true hernias deserve a proper surgical evaluation.
Hernia repair is not only about closing an opening. The objective is to restore abdominal wall function, reinforce weak tissue when needed, and choose the most appropriate technique according to the type of defect. In selected patients, robotic surgery in Colombia or laparoscopic repair may offer important advantages, while in other cases open repair remains the most appropriate and durable option. You can also explore my full range of minimally invasive surgical services for related abdominal procedures.
Main types of hernia treated and how surgical planning changes in each case
Inguinal hernia: the most common groin hernia in adults
How inguinal hernias typically present
Inguinal hernias usually appear as a groin bulge, pressure sensation, or pain that becomes more noticeable with standing, coughing, exercise, or lifting.
From a clinical standpoint, symptoms may range from mild discomfort to progressive limitation in daily activity.
Surgical indication depends on symptoms, reducibility, progression over time, and the patient’s overall functional demands.
Why the repair strategy is not always the same
Not all inguinal hernias require the same operation.
Decision-making is based on whether the hernia is unilateral, bilateral, recurrent, or associated with prior groin surgery.
In many patients, minimally invasive repair offers important advantages, while in others an open approach may remain more appropriate depending on anatomy and surgical history.
Umbilical hernia: midline weakness around the navel
When an umbilical defect becomes clinically relevant
Umbilical hernias develop near the umbilicus when the fascia weakens in the midline.
Some remain small for a period of time, but others enlarge progressively or become symptomatic with strain, weight gain, or physical activity.
Repair is usually considered when the defect becomes painful, enlarges, or begins to interfere with abdominal wall function.
How this may overlap with midline abdominal wall weakness
In some patients, an umbilical hernia coexists with widening of the linea alba or generalized midline weakness.
That distinction matters because not every abdominal bulge is explained by a true hernia alone.
When both conditions are present, evaluation may overlap with rectus diastasis repair in Colombia as part of a broader abdominal wall assessment.
Ventral hernia: more than a defect in the anterior abdominal wall
Why ventral hernias require an abdominal wall perspective
Ventral hernias involve the anterior abdominal wall outside the groin and may affect midline or paraumbilical regions.
From a surgical standpoint, repair is not just about closing a gap.
It often requires restoring continuity, strength, and load distribution across the abdominal wall, especially in larger defects or patients with poor tissue quality.
When reconstruction principles may matter
Larger ventral hernias may require more than standard closure.
Mesh reinforcement, defect closure strategy, and reconstruction principles may all influence long-term durability.
In selected patients, this is also where robotic surgery in Colombia may add value through precise suturing and minimally invasive abdominal wall reconstruction.
Incisional hernia: hernia through a previous surgical scar
Why prior surgery changes the repair strategy
Incisional hernias develop through prior abdominal incisions and are often more complex than primary defects.
Scar tissue, prior mesh, altered planes, and tissue weakness may all affect how the repair should be performed.
Decision-making is based on defect size, location, symptoms, previous repairs, and the expected balance between durability and surgical morbidity.
Why open repair still remains important in selected patients
Not all incisional hernias should be treated through the same minimally invasive pathway.
Although laparoscopic and robotic techniques may be helpful in selected cases, open repair still remains the most appropriate option for some large, complex, or heavily scarred defects.
The safest operation is the one that best matches the anatomy and tissue condition—not simply the newest technology.
Recurrent and bilateral hernias: when prior repair or double-sided disease changes the plan
Why recurrent hernias require a different level of planning
Recurrent hernias deserve special consideration because previous repair may alter tissue planes, increase scarring, and limit the safest route for reoperation.
From a clinical standpoint, these are not simply “the same hernia again.”
The prior technique, current anatomy, and recurrence pattern all influence the new repair strategy.
How bilateral disease may influence a minimally invasive approach
Bilateral inguinal hernias are often well suited to a minimally invasive strategy because both sides can be evaluated and repaired through the same access pathway in selected patients.
If you would like to explore other related abdominal procedures within my practice, you can visit the complete surgical services hub.
Prefer a more patient-friendly explanation of symptoms and local evaluation?
Read the Spanish version on hernia surgery in Medellín
.
Clinical decision-making: when hernia surgery is recommended — and when it is not
When hernia repair is usually recommended
Symptoms and findings that support surgical repair
From a clinical standpoint, hernia surgery is usually recommended when the defect causes pain, pressure, activity limitation, progressive enlargement, or recurrent episodes of protrusion that interfere with daily life.
Surgical indication also becomes stronger when there is concern for incarceration, bowel obstruction, or progressive loss of abdominal wall integrity.
Decision-making is based on symptom burden, anatomical findings, and the expected long-term benefit of repair.
Why elective repair is often safer than waiting for complications
Many hernias tend to enlarge over time rather than resolve on their own.
Elective surgery generally allows better planning, better patient optimization, and lower overall risk than urgent surgery performed after incarceration or strangulation has already occurred.
For that reason, many patients benefit from evaluation and repair before the hernia becomes more complex.
When immediate surgery may not be necessary
Not all patients require immediate repair
Not all patients require surgery right away.
Small, minimally symptomatic hernias may sometimes be monitored in selected patients, particularly when symptoms are limited and the risk of progression appears low in the short term.
However, watchful waiting should not mean ignoring the problem.
It means structured follow-up, reassessment of symptoms, and understanding that the indication may change over time.
When symptoms may not justify surgery yet
A visible bulge alone does not automatically mean that surgery is urgent.
Decision-making is based on whether the hernia truly explains the patient’s symptoms, whether the defect is progressing, and whether the expected benefit of repair clearly outweighs operative burden.
This is especially important in small defects, incidental findings, or patients with competing medical risks.
When the right decision is to optimize first and operate later
Why timing matters in abdominal wall surgery
In some patients, the safest strategy is not immediate surgery, but preoperative optimization first.
Weight control, smoking cessation, management of diabetes, improvement of nutritional status, or treatment of active infection may all improve healing and reduce the risk of recurrence or wound-related complications.
Evidence suggests that proper timing can be as important as technical execution in achieving a durable repair.
Why surgical indication depends on risk–benefit balance
Surgical indication depends on more than the diagnosis itself.
It depends on whether the expected benefit in pain relief, abdominal wall stability, and complication prevention outweighs operative risk for that specific patient.
This is also why the same hernia may be treated differently in two different patients depending on anatomy, symptoms, prior operations, and overall clinical condition.
Why formal surgical evaluation matters before choosing a technique
The operation should be chosen after the indication is clear
The first decision is not whether the repair will be open, laparoscopic, or robotic.
The first decision is whether surgery is indicated at all, and what the hernia is actually doing from an anatomical and functional standpoint.
Only after that evaluation does it make sense to compare minimally invasive options, open repair, or related abdominal wall procedures such as rectus diastasis repair in Colombia when midline weakness overlaps with a true fascial defect.
How this fits within a broader surgical care pathway in Colombia
A structured evaluation helps determine not only whether surgery is needed, but also whether the patient is best served by standard laparoscopy, selected robotic surgery in Colombia, or open abdominal wall repair.
You can also explore the broader surgical services hub for related procedures and treatment pathways.
Prefer a more patient-friendly explanation of warning signs, symptoms, and local evaluation?
Read the Spanish version on hernia surgery in Medellín
.
Laparoscopic and robotic technology in hernia surgery
Modern hernia surgery is increasingly performed through minimally invasive techniques, but technology alone does not determine the best operation.
From a clinical standpoint, the priority is to match the surgical approach to the type of hernia, defect size, prior operations, tissue quality, and expected durability of repair.
Laparoscopic and robotic platforms can improve visualization and instrument control, especially in selected inguinal, ventral, incisional, recurrent, or bilateral hernias.
However, not every defect benefits from the same minimally invasive strategy, and not every patient requires robotic assistance.
- Enhanced visualization of fascial planes and abdominal wall anatomy
- Small incisions with reduced access trauma in selected patients
- Lower postoperative pain in many minimally invasive repairs
- Earlier return to daily activity in appropriate cases
- Evaluation of bilateral groin defects through the same access pathway in selected patients
- More precise suturing and mesh positioning in complex abdominal wall repairs when robotic assistance adds value
- Better alignment between technique and anatomy when the approach is chosen through structured clinical decision-making
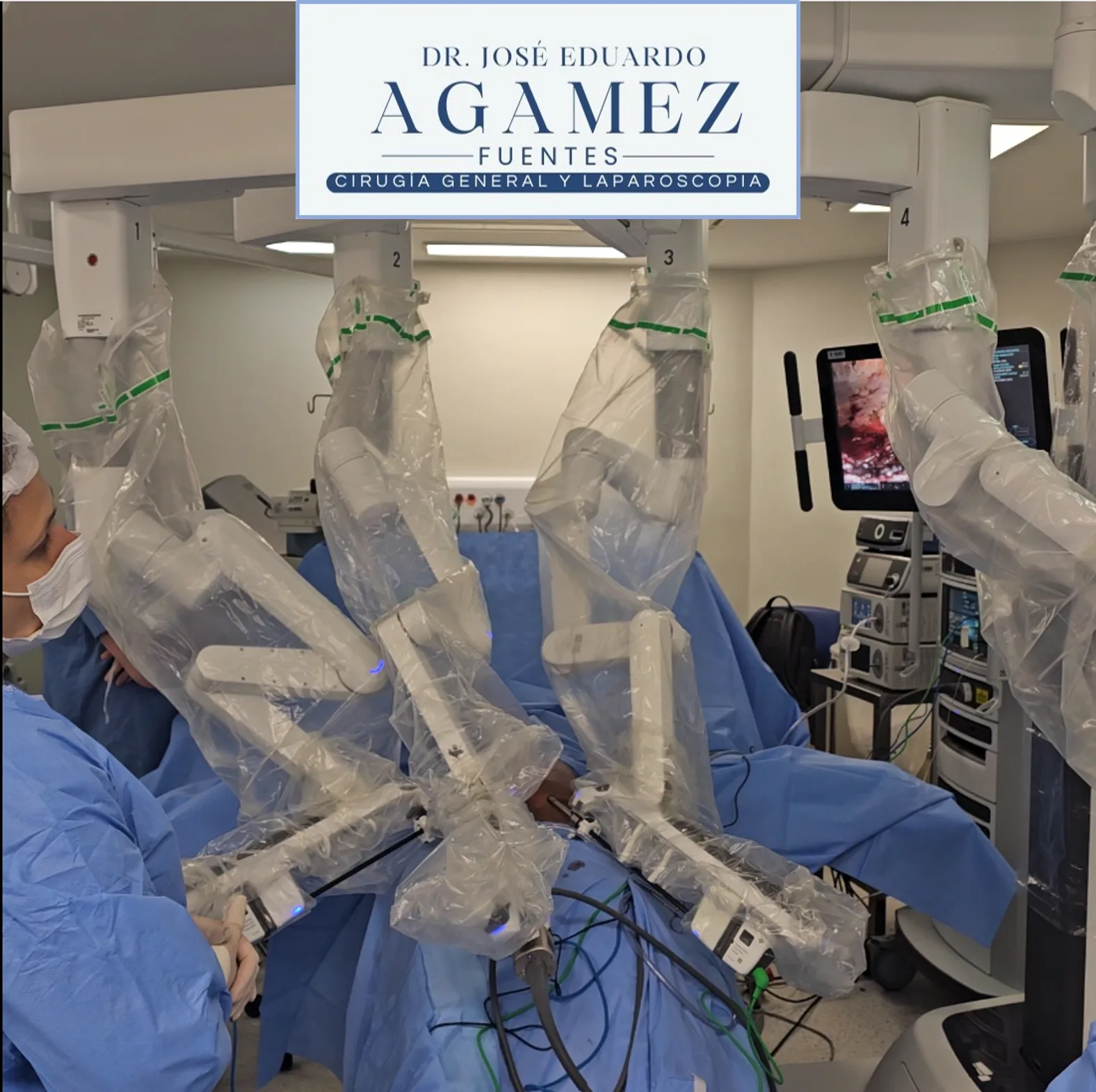
Robotic-assisted hernia surgery: when additional precision may be useful
Robotic technology can provide wristed articulation, stable three-dimensional visualization, and better ergonomics during selected abdominal wall repairs.
This may be particularly useful in some recurrent, bilateral, ventral, or incisional hernias where suturing, defect closure, or reconstruction strategy requires more refined instrument control.
Still, robotic surgery is not automatically superior for every patient.
Decision-making is based on complexity, anatomy, prior repairs, and whether robotic capability meaningfully improves safety or reconstruction quality in that specific case.
You can learn more about this broader approach on my robotic surgery in Colombia page.
Why open hernia repair still remains important in selected patients
Minimally invasive surgery is not the right answer for every hernia.
Some large defects, heavily scarred incisional hernias, or cases with challenging tissue conditions are better treated through an open approach.
From a surgical safety perspective, the best operation is not the least invasive one by default, but the one that offers the safest anatomical dissection, the most durable repair, and the most coherent risk–benefit balance for that patient.
For a broader view of related abdominal wall and minimally invasive procedures, you can also visit the surgical services hub.
Mesh repair and abdominal wall reconstruction in hernia surgery
Modern hernia repair is not only about closing a defect. From a clinical standpoint, it is about restoring abdominal wall strength, function, and long-term stability.
In many cases, this requires reinforcement of the repair using mesh and a structured approach to how the defect is reconstructed.
The objective is not just short-term closure, but a durable repair that reduces recurrence risk and preserves abdominal wall mechanics.
- Mesh reinforcement is commonly used to strengthen weakened fascial tissue and reduce recurrence rates
- Not all hernias require the same type of mesh or placement strategy
- Defect closure may be prioritized in some ventral or incisional hernias to restore abdominal wall continuity
- In larger defects, reconstruction principles may be required rather than simple repair
- Tissue quality, prior surgery, and hernia size all influence the repair strategy
- The goal is a balance between durability, safety, and preservation of abdominal wall function
Why not all hernia repairs should be approached in the same way
Not all hernias behave the same, and not all repairs should be performed with a single standardized technique.
From a surgical perspective, factors such as defect size, anatomical location, recurrence status, and tissue integrity determine whether the repair should prioritize closure, reinforcement, or full abdominal wall reconstruction.
A small primary hernia and a large incisional defect represent completely different problems, and treating them as equivalent can compromise long-term outcomes.
How mesh selection and placement influence long-term results
Mesh is not a single concept but a group of materials and placement strategies.
The decision depends on the type of hernia, the surgical approach, and the biological environment of the repair.
When properly indicated and correctly positioned, mesh reinforcement improves durability and reduces recurrence.
However, outcomes depend more on surgical planning and technique than on the material alone.
If you are exploring surgical options internationally, you can also review my profile on WhatClinic, where you can find additional information about minimally invasive procedures, patient pathways, and international care coordination in Colombia.